Background
Mental health disorders are one of the major public health issues worldwide with an estimated 970 million people (one in ten) living with a mental health condition globally (Dattani et al., 2021). One symptom that many, if not all mental health disorders have in common, are sleep problems (Dattani et al., 2021; NEDA, 2021; NHS, 2019; NHS, 2018). Research now shows that improving sleep has already been shown to improve physical health, overall health-related quality of life and even reduce healthcare costs (Scott et al., 2021; Sampson et al., 2021; Kyle et al., 2010; Espie et al., 2008). The most common sleep disorders are insomnias, an umbrella term for a variety of sleep disorders (DGSM, 2017; Spiegelhalder et al., 2011). Currently, cognitive behavioural therapy for insomnia (CBT-I) is recommended as the first-line treatment for chronic insomnia in adults of all ages (ESRS, 2017). Despite its relative effectiveness, the recent pandemic highlighted the necessity to have digital solutions for sleep (Jahrami et al., 2021). Current available digital solutions for sleep do exist, but tend to lack engaging features such as gamification. When considering that gamification is grounded in behaviour change theory, the delivery of fun & engaging psychoeducational content to improve sleep through mobile applications becomes viable.
Project Objectives
Therefore, the project aims to develop a digital solution, that combines aspects of gamificiation and education to help people improve their sleep and therefore there overall wellbeing and health mentally or physically.
Objectives:
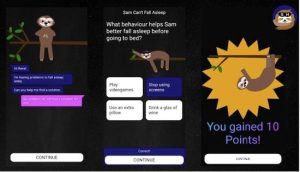
- Provide gamified digital solution to educate on healthy sleep behaviours
- Innovation: Benefits of gamification applied to digital sleep education
- Aim:
- Educate young adults on sleep
- help to achieve better sleep hygiene
- Improve sleep
- Improve health related quality of life and mental health
Evaluation
The fesability of this project was analyzed regarding its potential for further research and the development of a business case. SleepyHead creates value by offering instant digital access to gamified sleep education, that is engaging and easy to use. With our working prototype at hand and adequate resources, partners, channels, and activities there is a realistic opportunity to add to the currently limited field of research, which is the improvement of mental health and wellbeing through improved sleep using methods of digital gamified education. Larger studies will allow to reveal the true benefits of this approach and open further opportunities for the development of a viable business case. Especially considering the growing interest in refundable mobile health applications, like the health apps covered by German health insurances, the future will hold further opportunities to bring benefits of gamified sleep education to the greater public in an accessibly way.
Literature:
Dattani, S., Ritchie, H., Roser, M. (2021). Mental Health. Retrieved from: ourworldindata.org/mental-health [Online Resource].
DGSM – Deutsche Gesellschaft für Schlafforschung und Schlafmedizin. (2017). S3-Leitlinie Nicht erholsamer Schlaf/Schlafstörungen, Kapitel Insomnine bei Erwachsenen, Update 2016. Berlin: AWMF – Arbeitsgemeinschaft der Wissenschaftlichen Medizinischen Fachgesellschaften.
Espie, C. A., Fleming, L., Cassidy, J., Samuel, L., Taylor, L. M., White, C. A., Douglas, N. J., Engleman, H. M., Kelly, H. L., Paul, J. (2008). Randomized controlled clinical effectiveness trial of cognitive behavior therapy compared with treatment as usual for persistent insomnia in patients with cancer. Journal of clinical oncology: official journal of the American Society of Clinical Oncology, 26(28), 4651–4658. doi.org/10.1200/JCO.2007.13.9006
ESRS – European Sleep Research Society. (2017). European guideline for the diagnosis and treatment of insomnia. Regensburg: European Sleep Research Society.
Jahrami, H., BaHammam, A., Bragazzi, N., Saif, Z., Faris, M., Vitiello, M. (2021). Sleep problems during the COVID-19 pandemic by population: a systematic review and meta-analysis. Journal of Clinical Sleep Medicine, 17(2), 299-313. doi.org/10.5664/jcsm.8930
Kyle, S. D., Morgan, K., Espie, C. A. (2010). Insomnia and health-related quality of life. Sleep medicine reviews, 14(1), 69–82. doi.org/10.1016/j.smrv.2009.07.004
NEDA – National Eating Disorders Association (2021). Warning Signs and Symptom. Retrieved from: www.nationaleatingdisorders.org/learn/by-eating-disorder/anorexia/warning-signs-symptoms [Online Resource].
NHS – National Health Service (2018). Signs of an anxiety disorder. Retrieved from: www.nhs.uk/mental-health/feelings-symptoms-behaviours/feelings-and-symptoms/anxiety-disorder-signs/ [Online Resource].
NHS – National Health Service (2019). Symptoms – Bipolar disorder. Retrieved from: www.nhs.uk/mental-health/conditions/bipolar-disorder/symptoms/ [Online Resource].
Sampson, CJ., Bell, E., Cole, A., Miller, CB., Rose, J. (2021). Digital cognitive behavioural therapy for insomnia and primary care costs in England: an interrupted time series analysis. medRxiv 2021.
Scott, A. J., Webb, T. L., Martyn-St James, M., Rowse, G., Weich, S. (2021). Improving sleep quality leads to better mental health: A meta-analysis of randomised controlled trials. Sleep medicine reviews, 60, 101556. doi.org/10.1016/j.smrv.2021.101556
Spiegelhalder, K., Backhaus, J., Riemann, D. (2011). Schlafstörungen – Fortschritte der Psychotherapie (Band 7). Göttingen: Hogrefe.




